Welcome Clubfoot Families
“We at SCFAS want you to know that you are not alone, and we are here to help in any way we can. We understand how emotional the treatment process can be. The birth of any baby can trigger a host of emotions, from pure happiness to fear and anxiety. If you have just had a prenatal clubfoot diagnosis or are a parent of a child born with clubfoot, please know that clubfoot is a treatable birth defect, and it is completely normal to feel overwhelmed and scared while thinking about the future. If you plan to or have adopted a child with clubfoot, congratulations! You will be embarking on one of the most amazing experiences in your life by providing your child with a completely different life, starting with the use of their feet! Also, know that there is great hope for older children with clubfoot. We also welcome other loved ones and family members! Your family will be experiencing a potentially very challenging but equally rewarding process, and it is important to stay positive and supportive throughout this time. We are always happy to see family members at our appointments to help out or take pictures of the progression. We believe that the single most important thing we can do is provide you all with knowledge and reassurance to help give you confidence.
Studies show that informed parents and families will have better outcomes. On the following page, you will find information about clubfoot that will hopefully inform and reassure you. We also provide you with different clubfoot journeys that take you through the casting and bracing process in our before and after section. We want to thank our incredible families for sharing their photographs and perspectives to spread awareness that clubfoot is treatable.” Warm Regards,

Understanding Clubfoot: What Every Parent Needs to Know
Clubfoot is a congenital condition where one or both of a baby’s feet are twisted inward and downward. This affects the ability to stand or walk normally. Clubfoot is often identified at birth and can affect one or both feet. This condition can range in severity, but with proper treatment, most children can lead normal, active lives.
Types of Clubfoot
There are several types of clubfoot, each with distinct characteristics:
- Idiopathic Clubfoot
The most common form of clubfoot accounts for the majority of cases. The exact cause of idiopathic clubfoot remains unclear, though genetic and environmental factors may play a role. - Neurogenic Clubfoot
This form is caused by neurological conditions, such as spina bifida or cerebral palsy, which impact muscle development and coordination, leading to the development of clubfoot. - Syndromic Clubfoot
Often associated with other congenital syndromes, syndromic clubfoot occurs when clubfoot is one of several physical anomalies linked to genetic disorders or chromosomal abnormalities.

Causes of Clubfoot
The exact cause of clubfoot remains unclear, but there are several contributing factors that may increase its risk. Genetic predisposition and environmental influences can both play a role in its development. Additionally, neurological conditions such as spina bifida or cerebral palsy can also contribute to the condition. Ongoing research continues to explore the combination of genetic and environmental factors that may trigger clubfoot.
Treatment Options for Clubfoot
Ponseti Method
The Ponseti method is the most widely used treatment for clubfoot. This non-invasive technique involves gently manipulating the foot into the correct position and then applying plaster casts over several weeks to gradually adjust the foot. The Ponseti method has a high success rate, making it a preferred approach for many doctors and families.
Minimally Invasive Procedures
For some cases, minimally invasive procedures such as the Achilles tendon lengthening procedure may be recommended to further correct the foot position. Bracing is also an essential part of treatment to prevent relapse.
Bracing and Ongoing Care
A key aspect of clubfoot treatment is the use of braces after the initial casting phase. Parental discipline in maintaining the bracing schedule is crucial for ensuring long-term success. Over the years, the frequency of bracing gradually reduces, but adherence to this schedule is essential for preventing relapse.
Life After Clubfoot Treatment
After successful treatment, children with clubfoot can lead normal, active lives. Early intervention plays a crucial role in the outcome of clubfoot treatment, ensuring the best possible results. In addition to the Ponseti method or other treatments, physical therapy is often recommended to enhance strength and coordination as the child grows.
While most children recover fully, some may experience residual stiffness or muscle weakness. However, with ongoing care and physical therapy, these issues can often be managed, ensuring that your child can lead a life without limitations.
Support and Community for Clubfoot Families
At SCFAS, we believe that support and community are vital components of the clubfoot treatment journey. We invite families to become part of our SCFAS Clubfoot Club, where you can connect with others navigating similar challenges. Our support group meetings and special events, including the annual World Clubfoot Day celebration, provide valuable opportunities to share experiences and find encouragement.
Informed and connected parents are key to achieving the best outcomes for children with clubfoot. Join our community and find the support you need for this important journey.
Contact Us: Get Started on Your Clubfoot Treatment Journey
If your child has been diagnosed with clubfoot, early diagnosis and treatment can make all the difference. Our expert team, led by Dr. Nitza Rodriguez, is ready to help guide your family through the treatment process with compassion and expertise.
Contact us today to schedule a consultation and start your journey towards a brighter, more mobile future. Let us help you take the first step toward transforming your child’s life.

Contact Our Clubfoot Expert
Courtney Winger
For any questions or to discuss your child’s clubfoot diagnosis and treatment options, contact our expert at the following:
Phone: (949) 364-9255 ext: 1008
Direct Line: (949) 269-7558
E-Fax: (949) 238-7860
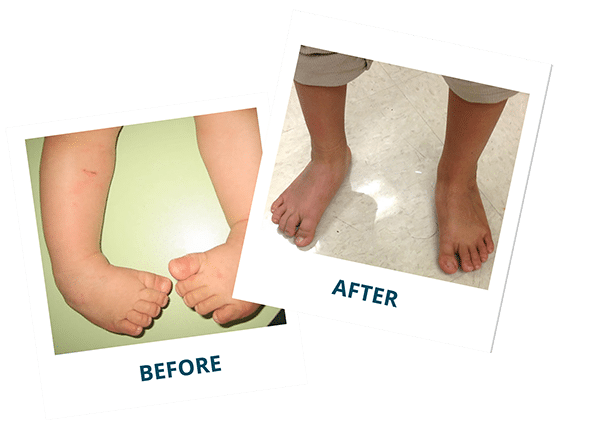
REAL KIDS, REAL RESULTS
FAQs
What is clubfoot
Congenital means it is present at birth. Talipes pertains to the foot and ankle, and Equino refers to the sagittal deformity or the tightness of the heel cord (Achilles tendon), causing the foot to point downward. The Varus refers to the frontal plane deformity in which the heel turns inward. Research shows that the condition develops in the womb around the third month of pregnancy and may be diagnosed on prenatal ultrasound. The condition can be unilateral (affecting only one foot) or bilateral (affecting both feet). The affected foot and calf are generally smaller in size than their unaffected counterparts. Clubfoot is one of the most common birth defects, affecting about 1 in 1000 newborns. Clubfoot can be flexible or rigid in nature and can cause significant pain and disability if left untreated. However, in newborns and non-ambulating babies, clubfoot is not painful.
When is clubfoot diagnosed?
Most cases of clubfoot are diagnosed at birth. Some cases are diagnosed through a routine prenatal ultrasound.
What causes clubfoot?
The cause is still unclear; therefore, the condition is sometimes referred to as idiopathic (unknown). We do know that there may be a genetic component and there is a higher incidence with a family history of clubfoot. Clubfoot can be associated with other abnormalities or exist by itself.
What is the treatment for clubfoot?
The gold standard for treating clubfoot is the Ponseti casting technique, developed by Dr. Ponseti in 1948. This is a method of serial gentle manipulations with application of plaster casts (5-7) above the knee to retain the correction. Weekly manipulations should ideally begin shortly after birth to facilitate the maximum advantage of soft tissue stretching and correct bone alignment. Before the last cast is applied, a minor procedure, Tendo Achilles Lengthening (TAL), is usually performed to lengthen the heel cord (Achilles tendon). The last cast will be worn for 3 weeks, thus allowing the tendon to heal completely. It is of utmost importance that parents be informed and understand that treatment does not end after the last cast. It is absolutely essential that a Foot Abduction Brace (FAB) be worn full-time for the first 3 months, slowly transitioned to only naps and nighttime until the child is 4-5 years old. This is necessary because, following correction, there is a high tendency of relapse, and the FAB is the only successful method for preventing a relapse when used consistently as described. X-rays are usually not necessary except in complicated cases.
A very small percentage of cases of clubfoot may be considered complex in which the foot is short, plump, stiff, and unyielding to stretching. These feet have a deep transverse skin fold above the heel and across the sole of the foot. These cases require special treatment and may need surgical correction. In general, for all cases of clubfoot, long-term studies show that bone and joint surgery should be avoided, since it leads to stiffness, scarring, and muscle weakness which become more apparent and disabling after adolescence.Can the Ponseti technique be used in older children?
Recent research shows that the Ponseti method can successfully be applied in children as old as ten. This is the case with neglected clubfoot, recurrent clubfoot, and even recurrent clubfoot in children with failed surgeries. The treatment for clubfoot should start as soon as possible, ideally within the first couple of weeks after birth.
How can you help eradicate clubfoot worldwide?
We at Southern California Foot and Ankle Specialists feel gratitude that the majority of infants born in the US have access to good care and therefore their clubfoot condition is corrected without causing severe limitations. However, clubfoot continues to be a serious problem in many developing nations. Neglected clubfoot is very debilitating, causing pain and severe disability, often ostracizing people and limiting their full potential as productive human beings. The Ponseti Method is a very practical option, as it is very cost effective and can be taught to local health providers to eliminate clubfoot disability.
Find out more on how we can come together and help eradicate clubfoot disability worldwide.

How to donate to clubfoot research?
Instructions for online gifts:
1. Enter amount of gift
2. Enter in “Other Designation” box: Dr. Dobb’s Research Fund
3. Click “Save Area and Amount” box
4. Proceed to next section

